In East Africa, including Burundi, haemophilia kills not only as a disease, but also through the absence of diagnosis, the shortage of medicines, and dependence on international donations. As climate disruptions weaken the cold chain essential to treatments, this rare condition is becoming a revealing indicator of the region’s healthcare vulnerabilities. For families, every unexpected bleed can turn into a tragedy, exposing children and adults alike to serious complications, lasting disabilities, and profound economic hardship.
By Ferdinand Mbonihankuye
“Haemophilia is a hereditary blood-clotting disorder caused by a deficiency in clotting factors,” explains Dr Stella Rwezaula, consultant haematologist at Muhimbili National Hospital and lecturer at the Muhimbili University of Health and Allied Sciences (MUHAS) in Dar es-Salaam, Tanzania. President of the Tanzania Haemophilia Society, she was speaking during a telephone interview about the medical and structural challenges posed by this rare disease in the region.
“The main symptom is prolonged bleeding that does not stop without treatment,” she continues. For families, it often begins with a period of confusion: a child who bleeds longer than expected, an adolescent whose knees swell painfully after minor knocks, or a patient whose bleeds recur repeatedly following a dental extraction.
A disease neither african nor European
In East Africa, haemophilia is sometimes described as a “foreign” or imported disease. This notion is medically unfounded. “Haemophilia affects all countries in the same way. It does not choose Africa or Europe,” explains Dr Rwezaula.
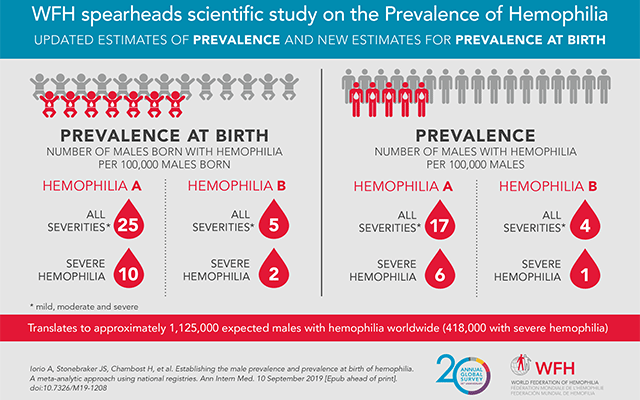
According to the World Federation of Hemophilia (WFH), approximately one person in every 10,000 lives with the disease worldwide. Haemophilia A, the most common form, affects one boy in every 5,000 male births, whilst form B affects approximately one in 25,000 to 30,000. These averages allow for an estimate of the theoretical number of cases in the region, often far exceeding registered figures.
In Tanzania, with more than 800,000 births per year according to the World Bank, approximately 160 new cases of haemophilia could appear annually. Kenya, the most populous country in the region with more than 1.3 million births per year, would account for more than 250 theoretical new cases.
In neighbouring countries, the figures are more modest but nonetheless significant: Rwanda (approximately 350,000 births per year) and Burundi (nearly 300,000) could each record 60 to 70 haemophilic boys annually — even though the vast majority are never diagnosed.
In reality, national registries record only a few dozen cases.
The World Federation of Hemophilia’s 2023 global report mentions fewer than 200 identified patients in Tanzania, fewer than a hundred in Kenya, and barely a handful of confirmed cases in Rwanda or Burundi.
This discrepancy alarms doctors. “Haemophilia is very much present here, but invisible in the statistics,” laments Dr Rwezaula. A lack of specialist laboratories, the cost of screening, and limited awareness of the disease all contribute to this invisibility. For as long as diagnosis remains a luxury, haemophilia will continue to be perceived as a distant disease — when in fact it is very much present here.
A genetic disease, but not exclusively male
Haemophilia is often described as a “male disease.” The explanation is genetic. “Haemophilia primarily affects men, as it is carried on the X chromosome,” explains Dr Rwezaula. Men have only one X chromosome: if it carries the mutated gene, the disease will manifest in its full form, in the absence of a back-up X chromosome.
Women generally carry one affected X chromosome and one functional X chromosome. In most cases, they are asymptomatic carriers. However, they are not entirely protected. “In rare cases, women may also be affected by haemophilia if both X chromosomes are mutated, or if the second X chromosome is inactive. This phenomenon is known as lyonisation,” Dr Rwezaula clarifies.
Treating the disease as “impossible” in women has consequences: female patients presenting haemorrhagic symptoms may be overlooked, misdiagnosed, or denied specialist care.
A disease That destroys in silence
The medical mechanism of haemophilia is straightforward to explain, yet it is devastating in practice. When the body lacks clotting factors, bleeding does not stop normally following an injury, surgery, or even a routine procedure.
“Circumcision can endanger the life of a boy with haemophilia,” states Dr Rwezaula. She notes that in mild forms, bleeding occurs mainly following trauma or surgery. In severe cases, it can occur spontaneously. “In severe haemophilia, patients can bleed even without any injury,” she adds.
More worryingly still, bleeding is not always visible. “Patients can wake up with bleeds in their joints or muscles,” she explains. Internal haemorrhages can be life-threatening, particularly intracranial haemorrhage. The gastrointestinal tract and urinary tract may also be affected, in which case patients vomit blood or present with blood in their stools or urine.
Haemophilia is therefore not merely a childhood disease. It is a chronic condition that can progressively damage the body, particularly when repeated joint bleeds cause chronic pain and deformities.
In Burundi, its lack of recognition has already claimed lives. Gilbert Niyonkuru, President of the Burundian Society of Persons with Haemophilia (Sobuh), speaks of this with restrained gravity. His commitment was born of personal tragedy.
“I visited almost every hospital in Burundi. Not a single healthcare professional was able to tell me what disease my child was suffering from,” he recounts.
For months, his son presented inexplicable symptoms. Consultations multiplied, without clear answers. Diagnoses wavered, treatments changed, but the child’s condition did not improve. Faced with this impasse, the father decided to cross the border.
He travelled to King Faisal Hospital in Kigali. There, doctors discovered a large haematoma on the child’s back, the consequence of a lumbar puncture carried out prior to cranial surgery. A clotting disorder was suspected.
“The doctors sent me to the University Teaching Hospital of Kigali (CHUK) to confirm or rule out the hypothesis,” he explains.
At that centre, the diagnosis was confirmed: type A haemophilia. Treatment was then initiated. With the support of the Rwanda Hemophilia Association and CHUK, the child began receiving Factor VIII, essential for blood clotting. Yet the relief remained precarious.
“I had to transport my son to Kigali every time he had an episode. Whether it was morning or evening, whether it was raining or the middle of the night, I had to cross the border,” details Niyonkuru.
After lengthy negotiations, the Rwandan doctors agreed, exceptionally, to provide him with a small supply of clotting factors, subsequently stored at Muyinga Hospital. A precarious arrangement, dependent upon goodwill and available stocks.
Then came the Covid-19 pandemic. Borders closed. Travel became impossible. “The doctors could not allow me to take medicines back to Burundi,” he says. His son died at the age of four.
Gilbert Niyonkuru, president of Sobuh (Burundian Society for People with Haemophilia). Photo credit: Ferdinand Mbonihankuye.
In 2022, devastated by this loss, Gilbert Niyonkuru founded the Burundian Society of Persons with Haemophilia, Sobuh, officially registered with the Burundian Ministry of the Interior.
Between medical ignorance and mystical accusations
“Without treatment, a patient can bleed to death,” warns Dr Rwezaula. When a child continues to bleed after a minor injury, many families in Burundi and East Africa do not think of a rare genetic disease. They think instead of witchcraft and a curse.
Several hundred kilometres from Muyinga, in the Jabe neighbourhood of Bujumbura, Blandine Kabanegeye does not contradict this observation. She revisits the early years of her son’s illness. Seated in her living room, she recounts a gradual descent into incomprehension.
“My son was under six years old when I noticed the first signs. He had bruises all over his body. His knees were swelling,” she recalls.
At the hospital, doctors initially suggested blood infections. Medicines were prescribed. Dietary advice was given. Nothing changed. Three months later, the symptoms returned, more severe.

Blandine Kabanegeye, mother of a child with haemophilia: ‘The family spends almost all its money on treatment.’ Credit: Ferdinand Mbonihankuye.
A doctor then proposed surgery to drain the fluid accumulated in the knee. In the operating theatre, however, surgeons discovered not fluid, but blood. The wound healed poorly. Bleeding persisted. The child’s condition deteriorated. “The doctor did not really know what was wrong with my son,” she says.
Around her, explanations took a different turn. Some spoke of a hex. Others of the wrath of ancestors. Her community accused her.
“We tried everything. Incantations, herbal baths, amulets. Nothing worked,” she confides.
Years passed. The family’s savings were exhausted. Eventually, the mother found more specialist medical support at the Polyclinique Centrale in Bujumbura, and then at the Roi Khaled Hospital. In-depth examinations were carried out.
The diagnosis was made: haemophilia. But the delay in treatment had left lasting damage. As a result of repeated joint bleeds, the child struggled to walk. He had to repeat his third year of primary school, unable to attend regularly.
As with the Niyonkuru family, Blandine Kabanegeye’s story reveals the failings of a system in which haemophilia remains poorly understood, frequently confused with other conditions, and sometimes interpreted through the prism of cultural beliefs.
“There is no specialist laboratory in the country. Basic coagulation tests are insufficient to confirm haemophilia and determine its type. There are no specialist doctors nor equipped laboratories to differentiate between haemophilia A and B, nor any medicines. The risks are numerous: loss of patients or permanent joint disability. Out of more than 2,000 patients that the association should be able to register according to birth prevalence, we count only 19, of whom 18 are alive and one has died,” states Mr Niyonkuru.
A financial abyss for families
For Burundian families, haemophilia is not merely a medical ordeal. It is an economic catastrophe. A single injection of clotting factor can amount to several hundred dollars, in a country where the average monthly income is approximately twenty dollars.
Mrs Kabanegeye describes an exhausting daily routine, punctuated by visits to the hospital up to three times a week. “We were eating only one meal a day,” she confides, her voice subdued. Her son, compelled to repeat his third year of primary school, cannot even make his own way home during a crisis. “His classmates carry him on their backs to the house when he has an episode,” she recounts.
Beyond the medical expenses that consume family savings, the disease deprives parents of any possibility of working. Maintaining income-generating activity is impossible when a child requires constant attention. “Burundi’s healthcare system is powerless in the face of haemophilia. No national registry exists, no monitoring is ensured. Patients must obtain treatments for themselves, often from abroad. The State concentrates its efforts on malaria, HIV, tuberculosis, and malnutrition,” laments Gilbert Niyonkuru.
Sobuh counts twenty-three members, predominantly men, largely children, in a country where the prevalence of haemophilia A is estimated at 1 case per 5,000. Clotting factor concentrates, donated by the World Federation of Hemophilia, are free but scarce.
The associated costs — transport, customs clearance, consultations, injections — combined with widespread poverty, impede access to medicines in Burundi. Without trained doctors or adequate equipment, late diagnoses worsen joint and haemorrhagic complications, and perpetuate social exclusion as well as early infant mortality, as noted by Mr Niyonkuru.
Population size matters
If the disease affects approximately one person in every 10,000 in Burundi, each country in East Africa should count hundreds of patients, whether diagnosed or not. “The number of patients depends on the size of the country’s population,” recalls Dr Rwezaula.
Diagnosis requires laboratory capacity concentrated in the capital and reference centres. “It requires coagulation tests, and many rural hospitals do not have them,” she notes.
“The majority of trained specialists are concentrated in national and tertiary hospitals,” she adds. The result is a pyramid-shaped system: a well-equipped apex in the capital, and a very broad base of under-resourced district establishments. For a disease in which early diagnosis can prevent disability and death, this configuration is catastrophic. Burundi is rarely mentioned in global debates on haemophilia, yet it almost certainly does not escape international estimates.
Treatment exists, but remains out of reach
Modern haemophilia care is among the great achievements of medicine. In high-income countries, patients live long lives with few complications, thanks to prophylaxis and regular access to factor concentrates.
In East Africa, these same medicines exist, but are rarely accessible. “Most African countries do not purchase factor concentrates because they are too expensive,” reports Dr Rwezaula. “The appropriate treatment consists of replacing the missing clotting factor. When factors are unavailable, we use blood products such as fresh frozen plasma. Cryoprecipitate may also be used, particularly for haemophilia A,” she explains. This, however, is a compromise. Blood products contain clotting factors in lower concentrations, which requires large volumes and repeated infusions. “They carry risks of transfusion-transmitted infections, particularly hepatitis and HIV,” she warns.
Dr Rwezaula also mentions the arrival of extended half-life treatments and factor-free therapies such as Emicizumab, administered subcutaneously and capable of preventing bleeds for several weeks, as well as gene therapy. However, access to these remains limited in Africa, she acknowledges.
Climatic changes affect storage
In debates on climate change and health, haemophilia is rarely mentioned. Yet it should be. The disease remains genetic — climate is not its cause. However, rising temperatures and energy instability threaten the systems that keep patients alive. This genetic disease requires treatment dependent upon a stable cold chain and continuous access to electricity — two resources that the climate crisis is rendering increasingly precarious.
The central issue is one of storage. “Factor concentrates must be kept between 2 and 8 degrees Celsius,” explains Dr Rwezaula. This presupposes functional refrigerators, a reliable electricity supply, and an intact cold chain from international transport to the patient. In many parts of East Africa, these conditions cannot be guaranteed.
Heatwaves, rising temperatures, and irregular electricity supplies further complicate storage. Some rural clinics have no refrigeration at all; hospitals suffer frequent power cuts, and patients live far from the centres that stock the concentrates. “The distance separating hospitals is a major risk, as haemorrhages are emergencies,” Dr Rwezaula underlines.
To address this, her team trains families in improvised cooling techniques using water and local materials, inspired by methods applied to other heat-sensitive biological products. The very fact that families must improvise, however, reveals the vulnerability of care in the face of climate shocks and energy insecurity.
Organisations such as the World Federation of Hemophilia and Health Care Without Harm are calling for these challenges to be integrated into climate policies. A study published in The Lancet Planetary Health underlines that global warming is already threatening blood supply chains and blood-derived products, making the construction of climate-resilient health systems a matter of urgency.
Up to $100,000 per patient per year
“Haemophilia is rare, but it is extremely costly,” continues Dr Rwezaula. Global estimates put the cost of treating a patient at approximately $100,000 per year in certain contexts. Even if this cost varies by country and model of care, the message is clear: treatment remains beyond the reach of the vast majority of families.
She observes that “families cannot afford to pay. Governments also struggle to meet the cost.” This is why donor support has become essential for haemophilia treatment in Africa. But this model is unsustainable. “We cannot rely on donors indefinitely,” she insists.
Dr Rwezaula’s warning takes on greater urgency when global policy is considered. International aid to health systems is evolving. In certain contexts, funding is diminishing, programmes are being restructured, and priorities are shifting.
For countries that depend on donations, the consequences are severe. “If donations decrease, the consequences for patients could be catastrophic,” she says. When factor concentrates cease to arrive, patients are not simply facing discomfort, but death. Hospitals revert to plasma transfusions, with a higher risk of infection. Families sell their possessions, children abandon school, and joint haemorrhages lead to lasting disabilities.
At Muhimbili National Hospital, Dr Rwezaula bears witness to the clinical burden of haemophilia. “The appropriate treatment consists of replacing the missing clotting factor,” she reiterates. Yet here again, “most African countries do not purchase factor concentrates because they are too expensive.” She reminds us that “many countries depend on donations,” particularly those from the World Federation of Hemophilia.
Gilbert Niyonkuru sums up the consequences for families. “Haemophilia creates enormous psychological distress and financially exhausts families, as patients must receive two to three injections per week without benefiting from free healthcare.” He calls for political action. “The government should provide the medicines necessary for the care of patients who remain in a critical situation owing to the lack of treatment.”
Sobuh, for its part, operates essentially through the contributions of impoverished families. It organises awareness sessions in schools, health centres, and through community radio. Yet reaching the entire country remains impossible with such limited means.
Collective purchasing
Dr Rwezaula’s recommendations are unequivocal. Governments must first begin purchasing factor concentrates, even progressively. “Regional bulk purchasing across East Africa could reduce costs,” she asserts. The decentralisation of diagnosis is equally indispensable. Coagulation tests must not remain confined to national hospitals, and healthcare professionals in every district must be trained to suspect and diagnose haemophilia. Finally, stigmatisation must be combated through public education. “Awareness-raising through the media, along with the training of patients and the wider community, is essential to reducing stigma,” she believes.
In Burundi — as has been established elsewhere in Tanzania, Kenya, and Uganda — the priorities are clear: develop a national strategy on rare diseases, introduce free healthcare for haemophilia patients, create equipped reference centres, establish a national patient registry, and conduct large-scale awareness campaigns.
“The government should provide the medicines necessary for the care of patients who remain in a critical situation owing to the lack of treatment,” urges Gilbert Niyonkuru.
Report produced with funding from the Ipsen Foundation. NPF is solely responsible for the content.